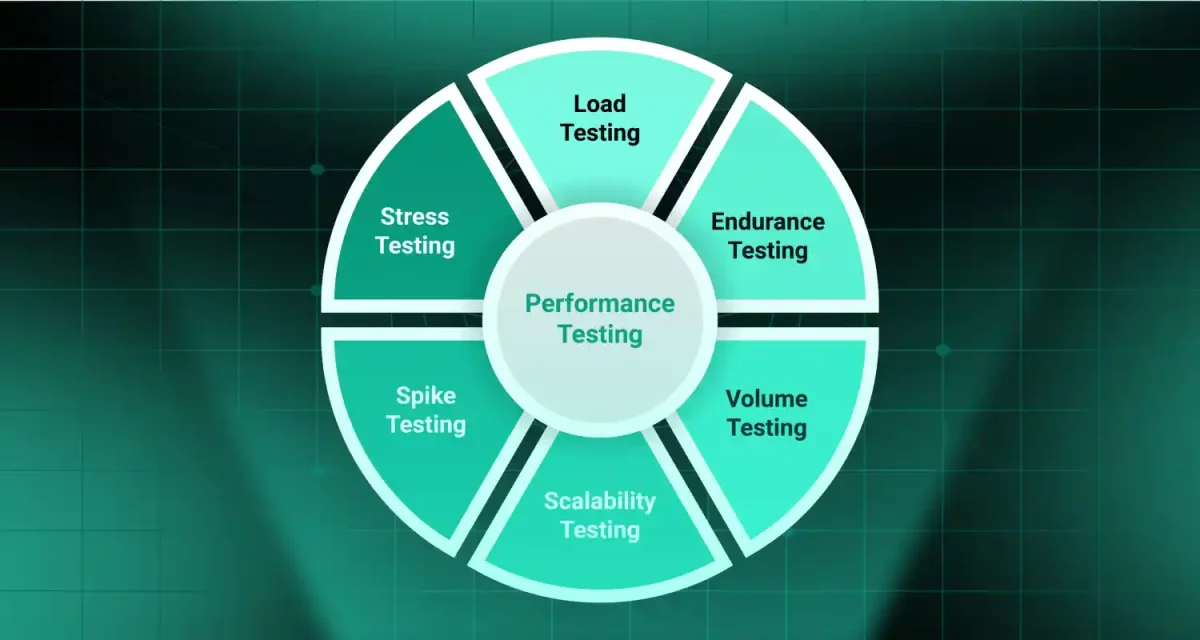
The healthcare landscape is evolving rapidly, with technology playing a central role in improving patient care and outcomes. At the heart of this is the Electronic Health Record (EHR), a comprehensive, digital version of a patient’s medical history, including diagnoses, treatments, medications, and more.
EHRs enhance care coordination and inform clinical decisions. With the explosion of patient data, EHRs are crucial for organizing and providing easy access to information. Interoperability, or seamless data exchange between healthcare systems, is essential for comprehensive patient care.
This article provides a step-by-step guide for healthcare professionals and organizations looking at how to build an EHR system. We’ll explore essential functions, implementation phases, and best practices.
1. Understanding the EHR ecosystem
A solid understanding of the EHR ecosystem is crucial for healthcare professionals and organizations considering building or implementing an EHR system. This section explores the key components and concepts of this ecosystem.
1.1. EHR vs. EMR: Clarifying the terminology
While often used interchangeably, Electronic Health Records (EHRs) and Electronic Medical Records (EMRs) have distinct differences. An EMR is a digital version of a patient’s chart within a single practice or facility. It primarily focuses on diagnosis and treatment. In contrast, an EHR is a more comprehensive record that spans across multiple healthcare settings, providing a holistic view of the patient’s health history. An EHR is designed to be shared with other healthcare providers, specialists, and even the patient, promoting better coordination of care.
1.2. The concept of patient-centered care and the EHR’s role
Patient-centered care places the patient at the heart of healthcare delivery, emphasizing their individual needs, preferences, and values. EHRs play a pivotal role in enabling this approach by providing a centralized repository of patient information, accessible to all members of the care team. This facilitates informed decision-making, personalized treatment plans, and improved communication between patients and providers. By empowering patients with access to their health information, EHRs also encourage them to take a more active role in managing their own health.
1.3. Benefits of EHR systems for various stakeholders
EHR systems offer numerous benefits:
- EHRs improve information sharing, reduce errors, prevent duplicate tests, and support clinical decision tools.
- By automating tasks and reducing paperwork, EHRs streamline workflows, shorten wait times, and decrease administrative costs.
- EHRs provide data for tracking outcomes, identifying trends, and improving care quality through advanced analytics.
- Long-term savings can be achieved through reduced paperwork, fewer errors, and improved billing practices.
2. Essential EHR functions and features
A modern EHR system is more than just a digital repository of patient information; it’s a powerful tool that transforms how healthcare is delivered. This section delves into the core functions that define an EHR system and the key software features that drive optimal performance, which is crucial in understanding how to build an EHR system.
2.1. Core functions of EHR systems
Understanding the eight core functions of EHR systems is fundamental to building comprehensive software:
- Patient identity and demographic data management
- Clinical documentation and charting
- Medication management and e-prescribing
- Order entry and results management (e.g., lab, radiology)
- Clinical decision support systems (CDSS)
- Patient engagement and communication tools
- Reporting, analytics, and population health
- Billing and financial management
2.2. Key EHR software features for optimal performance
In addition to the core functions, several key software features contribute to the performance and usability of an EHR system:
- Intuitive user interface and workflow customization
- Interoperability and data exchange capabilities
- Mobile accessibility and remote access
- Robust security and HIPAA compliance
- HL7 and FHIR standards

3. How to build an EHR system: A step-by-step guide
EHR system development is a complex undertaking that requires careful planning, execution, and ongoing management. This section provides a step-by-step guide to building an EHR system, helping healthcare organizations navigate this process successfully.
3.1. Phase 1: Planning and requirements analysis
The first phase sets the foundation for the entire project.
- Defining organizational goals and objectives: Clearly articulate what the organization aims to achieve with the EHR system. This could include improving patient care, increasing efficiency, reducing costs, or enhancing regulatory compliance.
- Conducting a comprehensive needs assessment: Evaluate the current state of the organization’s IT infrastructure, workflows, and data management practices. Identify the specific needs and pain points that the EHR system should address.
- Stakeholder engagement and requirements gathering: Involve all relevant stakeholders, including physicians, nurses, administrative staff, and patients, in the planning process. Gather their input on the desired features, functionalities, and usability of the EHR system.
- Budgeting and resource allocation: Develop a detailed budget that includes the cost of software, hardware, implementation, training, and ongoing maintenance. Allocate sufficient resources, including personnel and funding, to support the project.

3.2. Phase 2: System selection or development
In this phase, the organization will choose an EHR system that aligns with its needs and goals.
- Evaluating commercial EHR solutions: Researching and comparing top EHR software solutions for healthcare providers. Consider factors such as functionality, scalability, interoperability, cost, and vendor reputation.
- Considering custom EHR development: For organizations with unique requirements, custom development may be an option. This involves building an EHR system from the ground up, which offers greater flexibility but also requires more resources and expertise.
- Vendor selection and contract negotiation: Select a vendor that best meets the organization’s needs and negotiate a contract that clearly outlines the terms of service, including implementation, training, support, and maintenance.
- System design and customization: Work with the vendor or development team to design the system architecture, customize workflows, and configure the software to meet the organization’s specific requirements.
3.3. Phase 3: Implementation and deployment
This phase involves putting the EHR system into practice.
- Developing an implementation plan: Create a detailed plan that outlines the timeline, tasks, responsibilities, and milestones for the implementation process. This plan should also include strategies for change management, risk mitigation, and communication.
- Data migration and conversion strategies: Determine how patient data will be transferred from existing systems to the new EHR. Develop a data migration plan that ensures data accuracy, completeness, and security.
- System configuration and testing: Install and configure the EHR system, and conduct thorough testing to ensure that it functions correctly and meets the organization’s requirements. This includes testing workflows, integrations, and security features.
- User training and change management: Provide comprehensive training to all users on how to use the EHR system effectively. Implement change management strategies to address user resistance, promote adoption, and ensure a smooth transition to the new system.
3.4. Phase 4: Optimization and maintenance
The final phase of EHR system development focuses on ensuring the long-term success of the software.
- System monitoring and performance optimization: Continuously monitor the EHR system’s performance, identify areas for improvement, and optimize its functionality to meet evolving needs.
- Ongoing support and updates: Provide ongoing technical support to users, and ensure that the EHR system is regularly updated with the latest software patches, security updates, and feature enhancements.
- Compliance and security audits: Conduct regular audits to ensure that the EHR system complies with relevant regulations, such as HIPAA, and that patient data is secure.
Want to Integrate Powerful IT Solutions into Your Business?
We provide tailored IT solutions designed to fuel your success. Let`s map out a winning strategy. Starting with a free consultation.
Contact Us4. Best practices for successful EHR implementation
Implementing an EHR system is not just about installing software; it’s about transforming healthcare delivery. To ensure a smooth and successful transition, healthcare organizations should adhere to the following best practices:
4.1. Ensuring data integrity and security
Data integrity and security are paramount in any EHR implementation. Organizations must implement robust measures to protect patient information from unauthorized access, loss, or corruption. This includes:
- Implementing strong access controls and authentication mechanisms.
- Encrypting sensitive data both in transit and at rest.
- Regularly backing up data and having a disaster recovery plan in place.
- Conducting regular security audits and vulnerability assessments.
4.2. Promoting user adoption and minimizing resistance
User adoption is crucial for the success of any EHR implementation. To minimize resistance and encourage adoption, organizations should:
- Involve users in the selection and implementation process.
- Provide comprehensive training and ongoing support.
- Customize the system to align with user workflows.
- Communicate the benefits of the EHR system clearly and address user concerns.
- Establish super-users who can provide peer support.
4.3. Achieving interoperability with other systems
EHR systems should be able to seamlessly exchange data with other healthcare systems, such as:
- Other EHR systems
- Health information exchanges (HIEs)
- Laboratories and pharmacies
- Medical devices
- This requires adherence to interoperability standards and the use of technologies like APIs.
4.4. Adhering to regulatory requirements
EHR systems must comply with various regulations, such as HIPAA, to protect patient privacy and security. Organizations should:
- Conduct a thorough assessment of applicable regulations.
- Implement policies and procedures to ensure compliance.
- Provide regular training to staff on regulatory requirements.
- Stay updated on changes in regulations and update the EHR system accordingly.
4.5. Health information technology considerations
EHR implementation requires careful consideration of the organization’s overall health IT infrastructure. This includes:
- Ensuring that the network infrastructure can support the EHR system.
- Selecting appropriate hardware and software.
- Developing a strategy for managing and maintaining the system.
- Planning for future technology upgrades and scalability.
4.6. Patient data management
Effective patient data management is essential for accurate and reliable EHRs. Organizations should:
- Establish clear policies and procedures for data entry, storage, and retrieval.
- Implement data quality checks to ensure accuracy and completeness.
- Develop a data governance framework to manage data access and use.
- Provide patients with access to their health information and tools to manage their data.
5. The bottom lines
EHR system development offers substantial rewards for healthcare organizations and patients. This guide outlined the essential steps on how to build an EHR system: planning, system selection, implementation, and ongoing maintenance. EHRs are transforming healthcare by improving patient safety, enhancing efficiency, and empowering patients.
Future trends include increased interoperability, cloud solutions, AI integration, personalized medicine, and mobile health. We encourage healthcare organizations to embrace EHRs.
For expert assistance with designing and implementing a tailored EHR system, contact Stepmedia today.